Reducing Specimen Rejection Rates: How Transport Quality Impacts Laboratory Performance
Every clinical laboratory faces the same frustrating reality: specimens that arrive compromised, degraded, or otherwise unsuitable for testing. Specimen rejection rates in clinical laboratories typically range from 0.3% to 5% depending on specimen type, collection method, and transport conditions. While those percentages may sound small, for a laboratory processing thousands of specimens daily, even a 1% rejection rate translates into dozens of failed tests, repeated collections, delayed diagnoses, and significant financial losses. The majority of these rejections are preventable, and transport quality is one of the most controllable variables in the equation.
Transport-related specimen rejections occur when samples are exposed to conditions during transit that compromise their analytical integrity. Temperature excursions, hemolysis from rough handling, delayed delivery beyond specimen stability windows, and broken chain of custody documentation all contribute to rejection rates that erode laboratory performance. For organizations managing outreach programs across multiple collection sites, the distance between specimen collection and laboratory analysis introduces risk at every stage. Understanding these transport-related causes and implementing targeted solutions is the most direct path to reducing specimen rejection rates and improving diagnostic outcomes.

1. Understanding Transport-Related Causes of Specimen Rejection
Specimen rejection does not happen in isolation. It is the end result of a failure somewhere in the pre-analytical workflow, and transport is where many of those failures originate. According to the CDC’s specimen collection and handling guidelines, proper transport conditions are essential to maintaining specimen integrity from the point of collection through laboratory receipt. When those conditions break down during transit, the specimen may become unsuitable for analysis before a technologist ever opens the container.
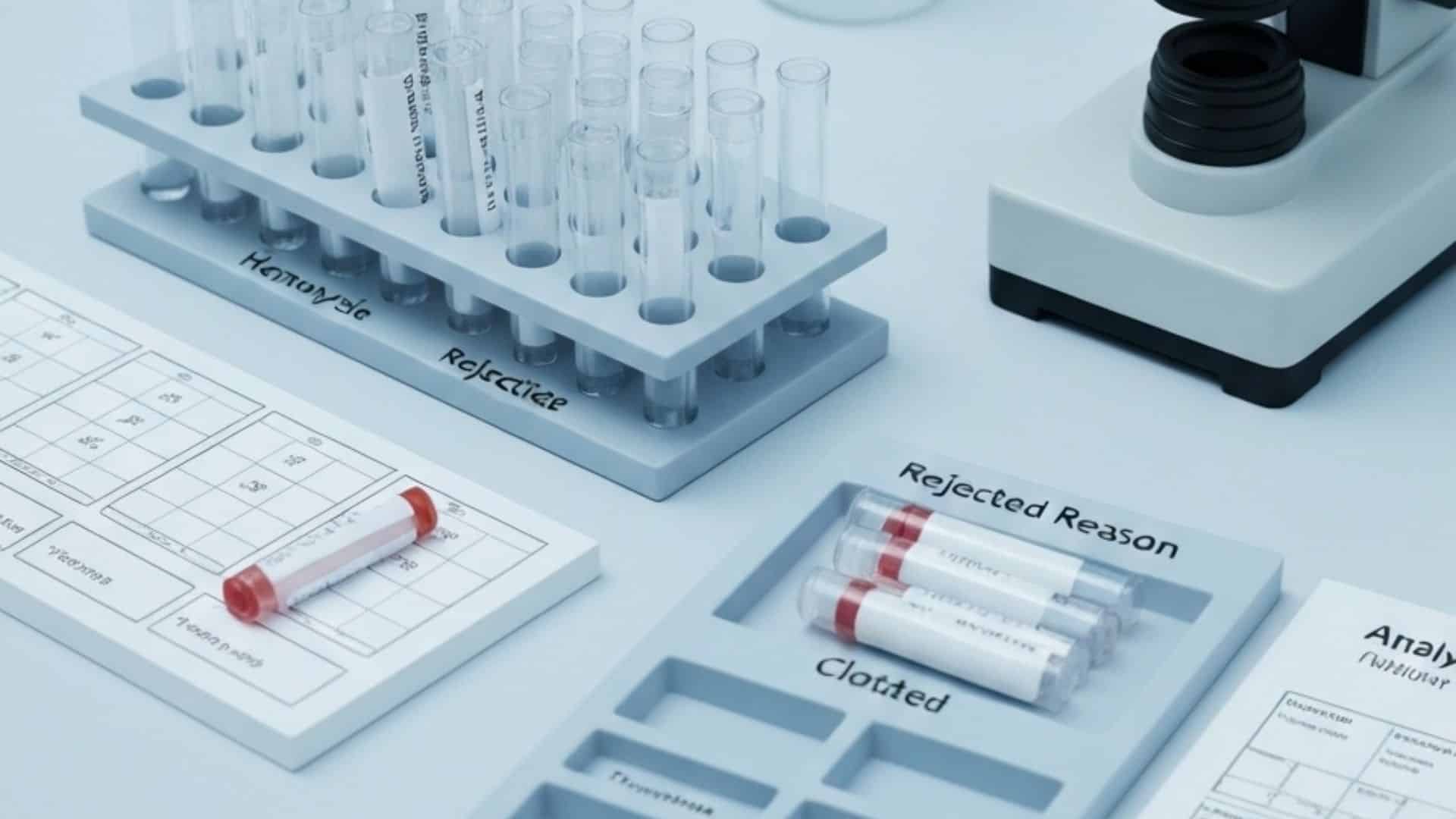
The most common transport-related rejection reasons fall into several well-documented categories. Hemolysis, the rupture of red blood cells that releases intracellular contents into serum or plasma, is the single most frequent cause of specimen rejection across clinical laboratories. While hemolysis can originate at the collection point, it is often caused or worsened during transport by excessive vibration, sudden temperature changes, or rough handling. Specimens that were viable at collection can become hemolyzed during a poorly managed transit, and the receiving laboratory has no way to distinguish collection-caused hemolysis from transport-caused hemolysis. The result is the same: the specimen is rejected, and the patient must undergo recollection.
Beyond hemolysis, pre-analytical errors during transport include clotted specimens that were not properly mixed or were held too long before transport, lipemic samples affected by temperature mismanagement, and insufficient volume specimens that result from partial leakage during transit. Each of these failure modes is directly linked to how the specimen was handled, packaged, and transported.
Primary Transport-Related Causes of Specimen Rejection:
- Hemolysis from excessive vibration, rough handling, or thermal shock during transit
- Temperature excursions that degrade analytes or trigger cellular changes in temperature-sensitive specimens
- Prolonged transit times that exceed specimen stability windows for time-critical analytes
- Clotted or partially clotted specimens caused by inadequate mixing or excessive hold times before pickup
- Leaking or compromised containers resulting from improper packaging or inadequate secondary containment
2. The Financial and Clinical Impact of High Rejection Rates
Specimen rejection rates are more than a laboratory quality metric. They represent a direct financial drain and a measurable threat to patient care. Every rejected specimen triggers a cascade of costs: the original collection and transport costs are lost, recollection must be scheduled, the patient must return for a new draw, and the laboratory must process the replacement specimen. Studies published by the American Society for Clinical Pathology (ASCP) have estimated that the total cost of a single rejected specimen, including recollection, repeat transport, reprocessing, and administrative overhead, ranges from $20 to over $200 depending on test complexity and specimen type.
For laboratories with high specimen volumes, even a modest reduction in rejection rates produces significant savings. A laboratory processing 5,000 specimens per day with a 2% rejection rate faces 100 rejected specimens daily. At an average cost of $50 per rejection, that totals $5,000 per day, or approximately $1.3 million annually, in avoidable waste. These are not hypothetical numbers. They reflect the documented cost of delivery errors in healthcare that laboratories absorb when transport quality is inadequate.
The clinical consequences are equally significant. Delayed test results postpone diagnosis and treatment initiation. For time-sensitive conditions, including sepsis workups, cardiac enzyme panels, and oncology molecular testing, even a 24-hour delay caused by specimen rejection can alter patient outcomes. The World Health Organization’s guidelines on the preanalytical phase emphasize that specimen integrity during transport is a foundational element of laboratory quality and patient safety.
Measurable Consequences of Elevated Rejection Rates:
- Direct financial losses from wasted reagents, consumables, and labor on specimens that cannot be tested
- Patient recall and recollection costs, including phlebotomy time, scheduling overhead, and repeat transport fees
- Delayed diagnosis and treatment for patients whose results are postponed by 24 to 72 hours
- Erosion of referring provider confidence that threatens outreach contracts and client retention
- Compliance exposure during CAP accreditation inspections where rejection rate trends are reviewed
3. How Temperature Monitoring and Cold Chain Management Reduce Rejections
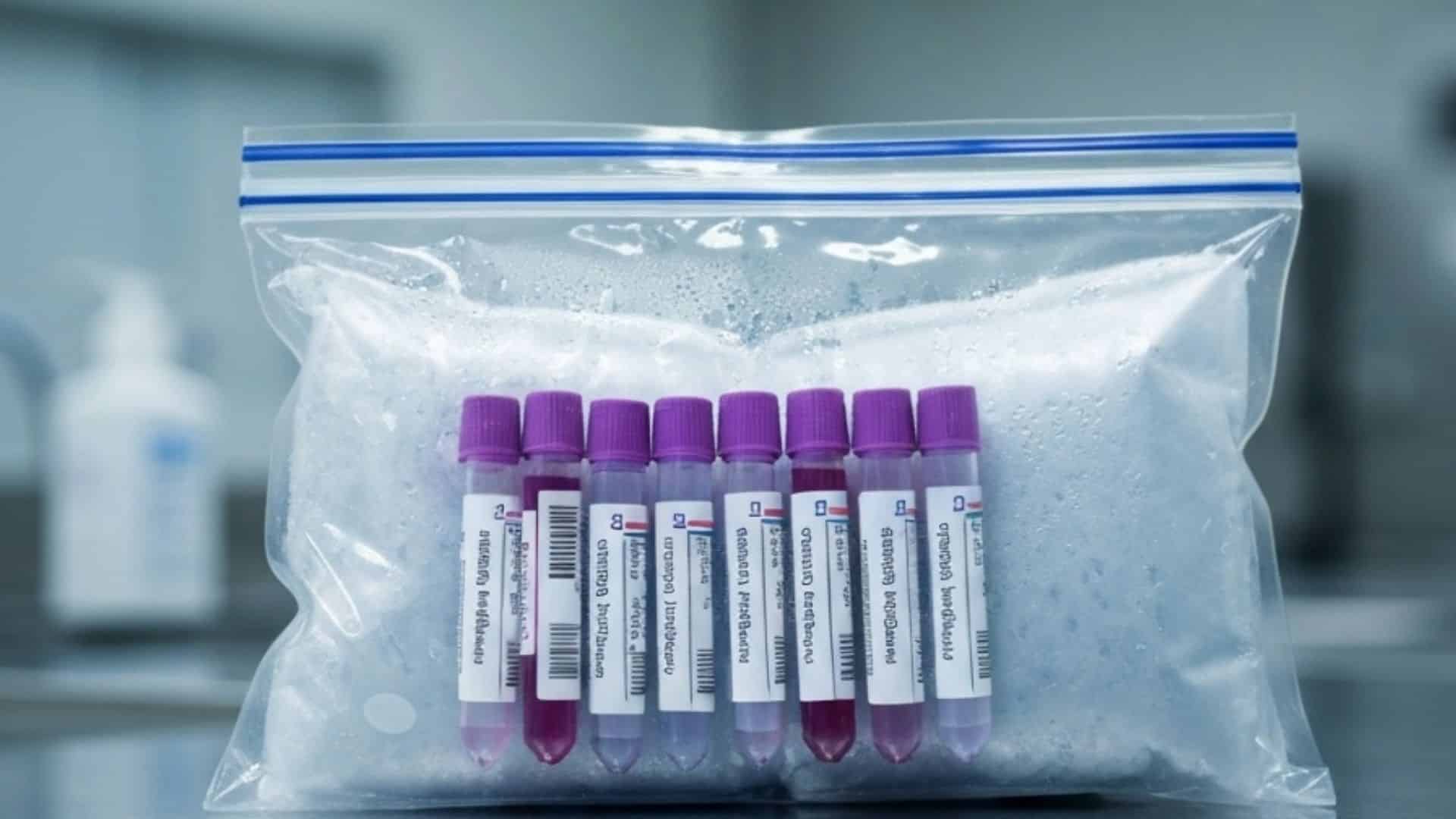
Temperature excursions during transport are one of the most preventable causes of specimen rejection, yet they remain one of the most common. The reason is straightforward: many courier services lack the infrastructure to maintain and document temperature conditions throughout the entire transport chain. A specimen that requires refrigeration at 2 to 8 degrees Celsius and spends 45 minutes in an unmonitored vehicle during summer heat may arrive within packaging that still feels cool to the touch, but the internal temperature may have exceeded acceptable thresholds long enough to compromise the analyte. Without continuous monitoring, neither the courier nor the laboratory can verify that conditions were maintained.
Effective cold chain logistics in healthcare require three components working together: validated packaging appropriate to the specimen’s thermal requirements, continuous temperature monitoring that records conditions at defined intervals throughout transit, and alert systems that notify logistics teams when temperatures deviate from the acceptable range. This approach, supported by temperature-controlled medical transport infrastructure, transforms temperature management from a hope-based system into a verified, auditable process.
The Clinical and Laboratory Standards Institute (CLSI) has established detailed guidelines for specimen transport temperatures across virtually every specimen type. Laboratories that align their courier requirements with CLSI standards and demand documented temperature compliance from their transport partners see measurable reductions in temperature-related rejections. The data is clear: when temperature conditions are continuously monitored and maintained, the rejection rate for temperature-sensitive specimens drops significantly.
Temperature Control Best Practices for Rejection Prevention:
- Continuous digital temperature logging throughout transport with timestamped records available to the receiving laboratory
- Validated packaging systems matched to specimen-specific thermal requirements across ambient, refrigerated, frozen, dry ice, and cryogenic ranges
- Automated threshold alerts that notify courier dispatch and laboratory staff when temperatures approach or exceed acceptable limits
- Seasonal transport protocols that account for extreme heat or cold conditions that affect packaging performance
- Post-delivery temperature verification at the laboratory receiving dock before specimens are accessioned into the testing workflow
4. Trained Medical Couriers vs. General Delivery Services
One of the most significant and least discussed contributors to specimen rejection rates is the difference between trained medical couriers and general delivery drivers. A general courier treats a specimen shipment as a package. A medical courier for laboratories understands that the container holds biological material with specific handling requirements, stability windows, and regulatory obligations. That distinction directly affects rejection rates.
Trained medical couriers understand why certain specimens must remain upright, why blood tubes should not be agitated during transport, why frozen specimens must be packed with sufficient dry ice to maintain temperature for the full transit duration plus a safety margin, and why chain of custody documentation must be completed at every handoff point. General delivery services do not train their drivers on these requirements because their business model is built around parcel logistics, not specimen science. The result is predictable: higher rejection rates, more temperature excursions, more handling-related hemolysis, and more documentation gaps that create compliance risk.
For laboratories managing lab outreach programs that depend on reliable specimen transport from dozens or hundreds of collection sites, the courier’s training level is directly correlated with specimen quality at receipt. Organizations that have transitioned from general delivery services to specialized medical courier providers consistently report measurable reductions in rejection rates, particularly for the transport-related rejection categories that general couriers are least equipped to prevent.
Capabilities That Distinguish Medical Couriers from General Delivery:
- Specimen handling certification covering proper orientation, vibration minimization, and biohazard protocols
- Knowledge of stability windows for different specimen types and the ability to prioritize time-critical pickups
- HIPAA, OSHA, and DOT compliance training with documented ongoing education requirements
- Understanding of packaging validation and secondary containment requirements for regulatory compliance
- Familiarity with CLIA and CAP specimen transport requirements that affect laboratory accreditation
5. Technology Solutions for Measuring and Reducing Rejection Rates
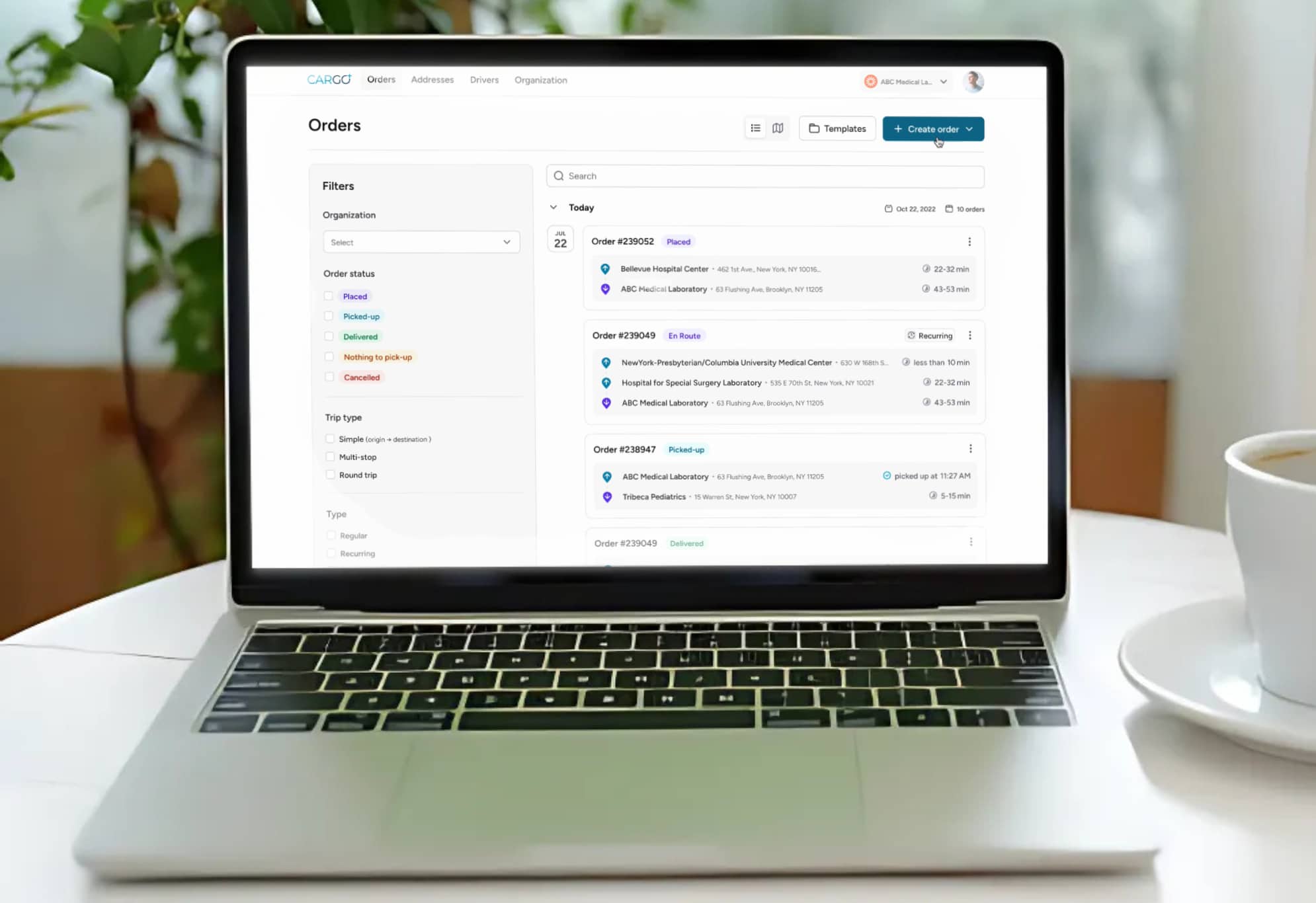
Reducing specimen rejection rates requires more than better packaging and trained couriers. It requires data. Laboratories and their transport partners need integrated systems that capture rejection data by cause, route, courier, specimen type, and time of day. Without this granularity, quality improvement efforts are based on assumptions rather than evidence. The most effective rejection reduction programs are built on analytics platforms that identify patterns, flag recurring failure points, and measure the impact of interventions over time.
AI-powered dispatch and routing systems represent a significant advancement in transport-related rejection prevention. Unlike static route planning that optimizes only for distance or stop count, intelligent dispatch systems account for specimen stability windows, real-time traffic conditions, weather-related temperature risks, and courier workload balancing. These systems ensure that a coagulation specimen with a two-hour stability window is not assigned to a route with six intervening stops. Real-time tracking provides visibility into every active specimen in transit, enabling proactive intervention when delays or route deviations threaten to compromise delivery within the stability window.
At carGO Health, our technology infrastructure is purpose-built for medical specimen transport. With over 200,000 orders completed, 98.9% on-time performance, and continuous temperature monitoring across all transport modes, our platform gives laboratories the data they need to track rejection rate trends and identify specific transport-related causes. Our AI-powered dispatch prioritizes time-sensitive specimens, and our certified medical couriers are trained in the handling science that general delivery services simply do not provide.
Technology Components That Drive Rejection Rate Reduction:
- AI-powered dispatch that routes specimens based on stability windows, priority level, and real-time conditions
- Continuous GPS tracking with estimated delivery times and automated alerts for delays or route deviations
- Integrated temperature monitoring dashboards that record and display thermal conditions throughout each transport
- Rejection analytics that categorize failures by cause, route, specimen type, and courier for targeted improvement
- Digital chain-of-custody platforms with barcode scanning, electronic signatures, and automated audit trail generation
- Client-facing reporting portals that provide laboratories with transparent access to transport quality metrics
Key Takeaways
Specimen rejection rates are a measurable indicator of transport quality, and transport quality is one of the most controllable variables in laboratory performance. By addressing the root causes of transport-related rejections, including temperature excursions, handling-induced hemolysis, excessive transit times, and chain-of-custody gaps, laboratories can achieve significant and sustained reductions in rejection rates. The financial savings from fewer recollections, the clinical benefits of faster and more reliable results, and the compliance advantages of documented transport quality all compound into a substantial return on investment.
The difference between laboratories that tolerate high rejection rates and those that systematically reduce them comes down to infrastructure: purpose-built transport systems, trained medical couriers, continuous monitoring technology, and data-driven quality improvement. These are not optional enhancements. They are foundational requirements for any laboratory that depends on outreach specimen logistics to deliver accurate diagnostic results.
If your laboratory is working to reduce specimen rejection rates and improve transport-related quality metrics, schedule a consultation to learn how carGO Health’s purpose-built medical courier infrastructure, AI-powered dispatch, and continuous temperature monitoring can protect specimen integrity across your entire collection network.
Frequently Asked Questions
What is an acceptable specimen rejection rate for clinical laboratories?
Most clinical laboratories target a specimen rejection rate below 2%, with best-in-class facilities achieving rates below 0.5%. The acceptable rate varies by specimen type and testing discipline. CAP accreditation requires laboratories to monitor and trend rejection rates as part of their quality management program, with documented corrective actions when rates exceed established thresholds.
How does transport quality affect specimen rejection rates?
Transport quality directly affects rejection rates through temperature management, handling technique, transit time, and chain-of-custody completeness. Specimens exposed to temperature excursions, excessive vibration, or prolonged transit beyond their stability windows arrive at the laboratory in a compromised state. Studies indicate that transport-related factors contribute to a significant percentage of all specimen rejections, making courier quality a primary lever for rejection rate improvement.
What is the most common reason for specimen rejection?
Hemolysis is consistently reported as the most common reason for specimen rejection across clinical laboratories, accounting for up to 60% of all rejections in some studies. Hemolysis can be caused by collection technique, but it is frequently worsened or caused by rough handling, excessive agitation, or thermal shock during transport. Proper courier training in specimen handling is one of the most effective interventions for reducing hemolysis-related rejections.
How do trained medical couriers reduce specimen rejections compared to general delivery services?
Trained medical couriers reduce rejections by understanding specimen handling science, including proper orientation, vibration minimization, temperature maintenance, and stability window awareness. They are certified in HIPAA, OSHA, and DOT compliance, and they follow established protocols for packaging validation and chain-of-custody documentation. General delivery drivers lack this specialized training, which results in higher rates of handling-related hemolysis, temperature excursions, and documentation gaps.
What role does temperature monitoring play in reducing specimen rejection rates?
Continuous temperature monitoring during transport provides verified documentation that specimens were maintained within required thermal ranges throughout transit. This monitoring enables real-time alerts when temperatures approach unacceptable thresholds, allows proactive intervention before specimens are compromised, and creates an auditable record for regulatory compliance. Laboratories that require continuous temperature monitoring from their courier partners consistently report lower rejection rates for temperature-sensitive specimen types.
Related Resources